July 2022
Fall Risk and Foot Problems in the Elderly
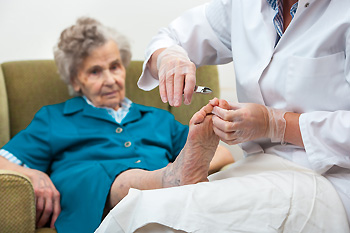
Foot problems in the elderly are a major concern because they contribute to balance and gait issues and lead to an increasing risk of falls. Seniors are physically weaker, have more mobility problems, and have reduced concentration than those that are younger. Their foot problems result from gait issues, poor posture, weakness of the bones, poor blood circulation, reduced sensation, inactivity, and fatigue. Since older people cannot always feel when they sustain an injury to their feet, they may develop wounds that are left untreated. Older people most often suffer from corns and calluses, bunions, foot fungus, hammertoe, toenail problems, and plantar fasciitis. If you are elderly or take care of one in this age group, it is suggested that you include a podiatrist on the health care team. If you, or the one you care for, notice ongoing problems or pain with feet and falling, a podiatrist can assess the situation and provide treatment.
Proper foot care is something many older adults forget to consider. If you have any concerns about your feet and ankles, contact Dr. Kirk Sherris from Liberty Bay Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
The Elderly and Their Feet
As we age we start to notice many changes in our body, but the elder population may not notice them right away. Medical conditions may prevent the elderly to take notice of their foot health right away. Poor vision is a lead contributor to not taking action for the elderly.
Common Conditions
- Neuropathy – can reduce feeling in the feet and can hide many life-threatening medical conditions.
- Reduced flexibility – prevents the ability of proper toenail trimming, and foot cleaning. If left untreated, it may lead to further medical issues.
- Foot sores – amongst the older population can be serious before they are discovered. Some of the problematic conditions they may face are:
- Gouging toenails affecting nearby toe
- Shoes that don’t fit properly
- Pressure sores
- Loss of circulation in legs & feet
- Edema & swelling of feet and ankles
Susceptible Infections
Diabetes and poor circulation can cause general loss of sensitivity over the years, turning a simple cut into a serious issue.
If you have any questions please feel free to contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Taking Care of Elderly Feet
Many foot diseases and conditions become more serious and common among the elderly. Some of these conditions include diabetic ulcers, ingrown toenails, fungus, arthritis, corns, and calluses. Unfortunately, it may be harder for older adults to take care of their own feet, but there are some precautions they can take in order to avoid any serious conditions.
Dry, cracked heels tend to be a common problem for older people. In order to avoid this, you should always keep your feet clean and well moisturized. Special feet moisturizers should be used as average lotions might not provide enough moisture for dry and cracked heels. Daily foot inspections are crucial for the elderly to detect any irregularities in their earliest stages. During the aging process, blood circulation tends to slow down causing older people to not feel their feet as well as they used to. This often results in foot problems going unnoticed.
Fungal and bacterial conditions thrive on elderly feet because older adults are less likely to keep their feet clean and dry; this makes it easier for bacteria to take hold in their dry, cracked skin. Elderly people should be sure to thoroughly dry their feet, especially in between the toes, after bathing. This will help them avoid developing any fungal infections. Additionally, clean cotton socks should be worn after the feet are dried.
Cutting toenails straight across will help prevent ingrown toenails. When toenails are cut too lose, the nail might break through the skin resulting in an ingrown nail. Clippers should be used to cut the nails in order to make the cut even.
Elderly people who have diabetes are at risk of developing serious foot problems that may lead to amputation. Ulcers that are left untreated can lead to gangrene. Dry and cracked feet, fungus, and untended cuts under the nails may also lead to infections.
Fortunately, Medicare covers many different types of services for foot care. Elderly people with any of these foot conditions should seek the help of a podiatrist and perform daily foot inspections in order to ensure that they have healthy feet.
Surgery for Ingrown Toenails
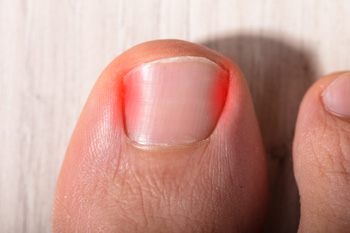
Ingrown toenails are unattractive and potentially uncomfortable foot ailments that primarily affect the big toenail. They occur when the side of the nail essentially grows into the skin of the toe. As a result, the affected area can swell, turn red, and become inflamed. There are many cases of ingrown toenails that, if caught early enough, can be treated and taken care of at home. Other cases can be addressed by a podiatrist with antibiotics or a splint and will not require surgery. However, if a case is severe enough and the ingrown toenail has become infected, then a surgery might be necessary to remedy the situation. There are a number of surgical procedures a doctor may perform. First, a doctor may perform a wedge resection (also known as a partial nail avulsion), in which a portion of the toenail causing the problem is removed. A doctor may also perform a toenail removal (or a complete nail plate avulsion) where the entire affected nail is removed. The intention behind this procedure is that the new nail will grow back correctly in 18 months. Of course, each patient’s potential to benefit from surgery for an ingrown toenail is highly individualized. As a standard rule of thumb, you can always consult with your podiatrist to determine the best treatment plan for your ingrown toenail.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Dr. Kirk Sherris of Liberty Bay Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ingrown Toenails
Ingrown toenails (onychocryptosis) are a common foot ailment and it is very unpleasant to experience. The condition is caused by an increase in pressure from the ingrowth of the nail edge into the skin of the toe. Ingrown toenails commonly cause pain in those who experience them. In some cases, the skin surrounding the ingrown toenail may break which may lead bacteria to enter through and cause an infection. Common symptoms of this ailment include pain, redness, swelling, and warmth around the toe.
An imbalance between the size of the nail and the enlargement of the nail skin edge causes ingrown toenails. This condition is often caused by improperly trimming the toenails. If you are trying you cut your nails, you should always try to trim straight across instead of in a rounded shape. Ingrown toenails can also be an inherited condition and they may also be caused by improper shoe fitting.
Another common cause of the condition is wearing shoes that are either too small or too large. Other causes include poor foot hygiene, obesity, diabetes, arthritis, edema, and fungal infections. There are many risk factors that may make a person more likely to develop an ingrown toenail. Athletes who play “stop and start” sports such as tennis, soccer, and basketball are most likely to have ingrown toenails.
People who have diabetes, a compromised immune system, or poor circulation should immediately seek care from a podiatrist if they have an ingrown toenail. It is also recommended to seek professional assistance if at-home remedies are not successful within a week or if there is persistent pain.
Why Live with Pain and Numbness in Your Feet?
Types of Foot Ulcers
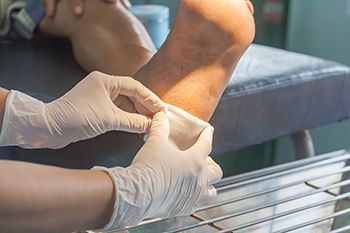
Patients who are diabetic may be familiar with wound care for the feet. Elevated blood sugar levels may cause a foot ulcer to gradually develop and immediate treatment may be necessary to avoid further implications, including amputation in severe cases. There are several types of foot ulcers that diabetic patients may experience. Neuropathy can cause a lack of feeling in the foot and patients are unable to feel the pain caused by an injury. A loss of blood flow to the feet can lead to an ischemic ulcer which can be difficult to treat. If the patient has poor circulation and neuropathy, a neuroischemic ulcer may form and it is said to be the most difficult to heal. Approximately half of foot ulcers become infected, therefore they need to be closely monitored. Diabetic foot ulcer treatment begins with removing infected tissue from the wound. This is called debridement and it is crucial in the prevention of damaged nerves, blood vessels, and tendons. This is followed by reducing existing pressure on the foot ulcer and draining the wound. If you have diabetes, it is strongly advised that you are under the care of a podiatrist who can treat and manage diabetic foot problems.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Kirk Sherris from Liberty Bay Foot & Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
How to Treat Your Toenail Fungus
While not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
What Is Causing My Toenail Problems?
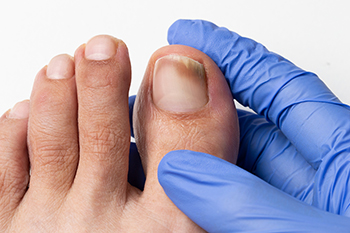
Toenails protect the toes. They are made of keratin, which makes them tough and resilient for the daily wear and tear they endure. Various things, including friction from ill-fitting shoes, level of physical activity, some pre-existing health conditions, temperature, and moisture, can affect toenails. Pain, itching, and discoloration are some of the signs of toenail problems. Toenail fungus, or onychomycosis, is a common toenail problem. It is more apt to affect older people, with half of all people over 70 developing a toenail fungal infection. It can also impact those who walk barefoot in public areas, like pool areas or locker rooms (with warm, dark, and damp conditions), and those who get sweaty feet or have diabetes. As the infection makes its way deeper into the toenail, the nail becomes discolored and thickened. The nail may crumble and become jagged at the edge. The infection can spread to other toenails and surrounding skin. If it oozes a foul-smelling pus, the infection is worse. It is important to see a podiatrist if you feel you have toenail fungus or any other troubling issues with your toenails. They can properly diagnose the problem and discern how it should be treated.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Dr. Kirk Sherris of Liberty Bay Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.







