May 2022
Determining the Cause of Your Heel Pain

There are many possible causes of heel pain, with plantar fasciitis being the most probable. This condition is an inflammation of the plantar fascia tissue on the bottom of the foot that connects the toes with the heel. This is where the pain is felt. Pain on the bottom of the heel may also be due to a stress fracture in the heel caused by repetitive stress. Pain at the back of the heel can be caused by several additional conditions. Heel bursitis occurs when the fluid-filled bursa sac at the back of the heel becomes irritated and inflamed. Haglund’s deformity is a bony enlargement at the back of the heel which can sometimes be caused by high-heeled, or hard-backed shoes that rub against the area. Achilles tendinitis is an inflammation of the Achilles tendon that also produces pain at the back of the heel where it attaches to the heel bone. Sever’s disease, which is an inflammation of the heel growth plate in growing children, can also cause pain in the back of the heel. A podiatrist is highly skilled at pinpointing the underlying issue causing heel pain and treating it accordingly. Make an appointment today if you are experiencing any kind of heel pain.
Many people suffer from bouts of heel pain. For more information, contact Dr. Kirk Sherris of Liberty Bay Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How Blisters on the Feet Can Be Prevented
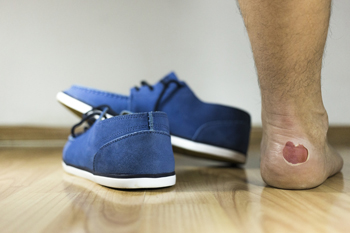
Many runners know the pain and discomfort of a blister on their feet while trying to walk or run. Most blisters develop from friction due to wearing shoes and socks that do not fit correctly which can damage the skin. At first, a blister looks like a bubble filled with liquid that protects the raw skin. When new skin has formed the blister will gradually drain on its own. To help prevent blisters from forming ensure running shoes fit correctly and observe the surfaces that you walk or run on. People who enjoy running marathons may be aware of blister prevention by using tape and adhesive on a specific area on the foot, followed by performing a test run to determine if it's placed properly. Runners find that having a blister on the foot changes the way their practice is done, and it can affect the biomechanics of the foot. It could lead to slower running, which may lead to running in the elements longer than expected. If you would like more information about blisters and their prevention, please confer with a podiatrist.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Dr. Kirk Sherris of Liberty Bay Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wounds That Don't Heal Need to Be Checked
Common Reasons Why Cracked Heels Develop
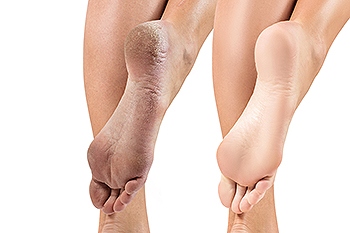
The most obvious reason a patient can get cracked heels is by having dry skin. Additional reasons that this uncomfortable foot condition can develop include standing on hard surfaces for long periods of time during the day, being overweight, and having foot problems that may increase heel pressure. It can happen to people who wear flip-flops or open backed shoes, which can cause the fat pads in the heel to expand sideways. Existing medical conditions may cause cracked heels. These can include psoriasis, eczema, or diabetes. Cracked heels can cause pain and discomfort, and may become infected if bacteria enters the body through the cracks. Effective prevention methods include wearing shoes that have a closed back and fit correctly, and frequently applying a good moisturizer throughout the day. Many people choose to wear padded socks which may help to prevent injuries to the affected foot. If you have cracked heels, it is suggested that you confer with a podiatrist who can guide you toward the treatment that is correct for you.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact Dr. Kirk Sherris from Liberty Bay Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Preventing Diabetic Wounds With Good Foot Care
Diabetes can impair a person’s ability to feel differences in temperature or pain in their feet. This is because high levels of blood sugar can cause nerve damage, or diabetic neuropathy. Any little cut, scrape, pressure point or disturbance in the skin that goes undetected has the potential of becoming a more serious wound. Wounds can be dangerous to a person with diabetes because their heightened levels of blood glucose can also restrict circulation in the feet and their body’s ability to heal itself. Daily foot care then becomes essential for the diabetic to stay healthy and to prevent wounds and infections from developing. Feet should be kept clean, but never washed with water hot enough to scald the skin. Moisturizing the skin will help keep skin healthy and prevent it from cracking. Toenails should be kept trimmed straight across, and not too short. Jagged or long nails may cut into skin on surrounding toes, and toenails that are rounded or too short may lead to ingrown toenails. Feet should be inspected at least once a day to make sure no trauma has occurred to the skin. If anything unusual is detected, it is suggested you consult a podiatrist right away. In fact, regular visits with your podiatrist will be an important part of maintaining foot health and preventing wounds and ulcers from developing.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Kirk Sherris from Liberty Bay Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Children Can Heal Quickly From Broken Bones

Research has shown that broken bones heal rapidly in children. Healing may take longer than several weeks, but new bones form soon after the fracture. During the inflammatory stage of healing, pain and tenderness often occurs. This is the signal the body uses to stop activity, as is the case in a broken foot. Blood clots form surrounding the affected area, and this is the first connection between the pieces of broken bone. A soft bone replaces the blood clot in the second stage, which is referred to as the reparative stage. This will gradually harden in approximately two to six weeks. The remodeling stage consists of hard bone that replaces the soft bone, or callus, and the broken bone will eventually become reshaped. It will appear to look and feel normal. If your child has broken their foot, please consult with a podiatrist for immediate medical care and proper treatment options.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Dr. Kirk Sherris from Liberty Bay Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our office located in Poulsbo, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.







